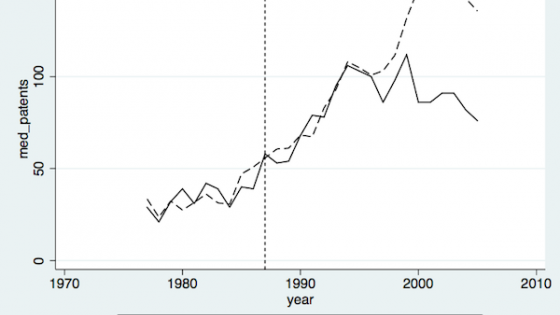A danger prominently voiced in public debates over the liability system is that large settlements arising from medical malpractice litigation lead doctors to practice ‘defensive medicine’ – that is, performing excessive tests and procedures because of concerns about malpractice liability. In the US, reform advocates typically contrast the high costs of defensive medicine procedures with their low expected benefits to patients, and a number of members of Congress support the idea that tort reforms capping physicians’ liabilities may reduce healthcare costs. This debate is also taking place in Canada, the UK, and Europe as increasing healthcare expenditure becomes a growing concern.
Since the 1970s, more than half of the states in the US have implemented some form of tort reform. A large number of academic studies have investigated the relationship between the tort system, treatment intensity, and medical expenditures. Many of these papers show that tort reforms may mitigate defensive medicine concerns by reducing treatment intensities (e.g. Kessler and McClellan 1996, Kessler 2011, Avraham and Schanzenbach 2015).
In addition to their effects on medical procedures and malpractice claims, tort reforms may also impact R&D investments and technological change. Parchomovsky and Stein (2008) and other law scholars have warned about a potential ‘chilling effect’ of the current tort system on innovation; that is, high damages and the court's reliance on custom may reduce physicians' willingness to adopt new, but riskier technologies, even if they are potentially superior to customary treatments. This idea that ‘product liability retards innovation’ has become a key argument for tort reform advocates, and has gained substantial ground over the years in courts and Congress. A typical counter-argument is that high liabilities may also encourage innovation because they induce physicians to ‘defensively adopt’ innovative technologies that are themselves safer or help physicians manage risks (e.g., monitoring devices and tests).
Despite these claims, the empirical literature on the relationship between liability risk and innovation is scarce. In recent research, we address this gap by studying the impact of tort reform on innovation in the medical device sector, a field of technology closely linked to malpractice litigation (Galasso and Luo 2016).
Tort reforms and medical device patenting
Our empirical work combines measures of innovation, based on US patent data, with information on state tort reforms from the American Tort Reform Association. We exploit the detailed technology classification system of the US Patent and Trademark Office (USPTO) to identify medical instrument patents. The USPTO data also provide information on the inventor address and the application year of a patent, which we use to trace medical device patenting activity across the US states for the period 1985-2005.
The class of tort reform central to our empirical analysis is the introduction of caps on non-economic damages – that is, damages other than monetary losses, such as pain and suffering. These damages typically comprise a substantial fraction of total awards and represent the main focus of tort reform advocates.
Our main result shows that patenting in medical instruments is reduced by roughly 14% in the presence of caps on non-economic damages. This negative effect suggests that, in the absence of these caps, the demand for new technologies that high liabilities generate through ‘defensive-adoption’ exceeds their negative ‘chilling effect’ on medical device innovation.
As an illustrative example, Figure 1 exemplifies how medical instrument patenting responded to the introduction of non-economic damage caps in Michigan and Utah. The figure compares innovation in these two states with innovation in a reference group of states without damage caps through our sample period. Patenting decreases relative to the comparison group after the states passed the reform, with the effect increasing over time and reaching a peak after five or six years. Our research documents similar effects for other sizable states introducing damage caps, and opposite effects for those states eliminating their damage caps during our sample period.
Figure 1 Tort reform and innovation
a. Michigan

b. Utah

In a variety of empirical tests, we show that our results are not driven by the largest states or the largest medical device innovators. We also investigated whether the policy change in one state affects medical device patenting in nearby states. We find very limited evidence of an effect on states that are geographically or economically close to states passing the reform. We conjecture that such a local nature of the policy impact is related to a key feature of the medical device industry – the involvement of practicing physicians. Indeed, a sizable fraction of the negative impact of tort reforms appears to be driven by the patenting activity of physician innovators located in the state.
Our research also shows that the negative effect of tort reforms is much more pronounced for patenting related to specialities with a high frequency of malpractice claims (such as surgery and orthopaedics). Conversely, caps on damages have a small and statistically insignificant effect on patenting in medical fields with few malpractice claims (such as dental and optics). Moreover, we document a non-monotonic U-shaped relationship between the effect of tort reforms and innovation quality. Caps on damages have no statistically significant effect on innovation at the lowest and highest quality levels. The effect is negative, statistically significant and of large magnitude for medical devices of intermediate quality.
Dynamic impacts of liability reforms
Our findings provide empirical evidence that tort reforms can affect the rate of technological change, indicating that these policies have dynamic effects on innovation incentives that go beyond their impact on patients and health costs. Recognising and estimating these dynamic effects is important when evaluating the costs and benefits of tort reforms, especially in technology fields characterised by a high frequency of liability claims.
While documenting an average negative effect of tort reforms on innovation, our research finds no effect for the most valuable medical technologies. This suggests that, on average, the development of breakthrough medical devices appears neither hindered nor accelerated by changes to the current liability system.
Our study does not find evidence for a significant chilling effect of liabilities on medical device patenting, but future research is warranted to further understand the relationship between liability and innovation across industries, technologies, and institutional environments.
References
Avraham, R and M Schanzenbach (2015) "The impact of tort reform on intensity of treatment: Evidence from heart patients", Journal of Health Economics, 39: 273-288.
Galasso, A and H Luo (2016) “Tort reform and innovation”, CEPR Discussion Paper No. 11358.
Kessler, D and M McClellan (1996) "Do doctors practice defensive medicine?", Quarterly Journal of Economics, 111: 353-390.
Kessler, D (2011) “Evaluating the medical malpractice system and options for reform”, Journal of Economic Perspectives, 25: 93–110.
Parchomovsky, G and A Stein (2008) "Torts and innovation", Michigan Law Review, 107: 285-315.