One of the most robust findings in the social sciences is the strong positive correlation between education and health status at all ages. There are many potential pathways that could explain why education plays a role in promoting better health. However, a positive association between education and health could also exist because the same observed and unobserved factors that determine educational attainment (for example, parental socioeconomic position, genetic ability, time and risk preferences) also determine health at birth and returns to investments in health. For this reason, establishing causality in the relationship between education and health is an important topic for researchers and policymakers alike.
The economics literature has sought to establish causality by exploiting policy reforms that increased compulsory years of education, tracing the effect of these increases on various measures of health and health-related behaviours in adulthood. The most commonly studied reforms are those that increased the minimum school leaving age. One strand of the literature has focused on the causal link between education and mortality. Another has examined measures of ill-health.
The results from this literature are mixed, giving rise to considerable disagreement about the extent to which education and health are causally related. Many studies find evidence that the additional year of schooling induced by these reforms drove significant improvements for some health or health-related behaviours (Lleras-Muney 2005 and Oreopoulos 2006 are early examples). But other studies, sometimes using the same data but different model specifications or measures of health, report little or no evidence of a causal effect (e.g. Clark and Royer 2013 for the UK, Meghir et al. 2018 for Sweden). Two recent reviews also come to different conclusions. Galama et al. (2018) conclude that there appears to be a causal effect of education on mortality and smoking but not on obesity, but even this is context specific. Hamad et al. (2018) conclude that education has a causal effect on most health outcomes.
Our contribution is twofold: first, we provide a comprehensive study of the causal link between education and a large set of prevalent chronic health conditions; and second, we look at the impact of increases in education at both the minimum school leaving age and further up the education distribution, which has been much less studied.
Chronic conditions (such as cardiovascular disease, diabetes, arthritis, back and neck pain, and mental health problems) are the main cause of poor health and disability in many countries. Worldwide the disease burden is shifting away from communicable to non-communicable diseases, with substantial implications for healthcare budgets. In England, for example, the treatment and care of people with chronic disease accounts for an estimated 70% of total health and social care expenditure.. Many chronic conditions result from lifestyle decisions (tobacco use, physical inactivity, excessive alcohol consumption and poor diet), all of which are potentially affected by greater education. So understanding whether education is causally linked to these conditions is important. However, there is relatively little robust evidence for many chronic conditions. The studies that exist have considerable variation in empirical specifications, sample sizes, the birth cohorts examined, and the measurement of health outcomes. Sample sizes in this literature have a median size of 28,310, which contrast with the much larger samples available to study the effect of education on mortality.
Our research (Janke et al. 2020) applies a consistent modelling approach to information on a wide range of chronic health conditions. We exploit two education reforms that affected large parts of the population.
The first is the 1972 raising of the minimum school leaving age from 15 to 16 years. It applied to cohorts born in or after September 1957 and affected around 25% of this population. These were individuals who would otherwise have left school at age 15. These individuals are now in late middle age, a time when many important chronic conditions have emerged.
The second is the large rise in British educational attainment that occurred around 1990. Whilst this was not a compulsory education reform, the outcome of a number of educational policy changes which occurred at the same time was to significantly increase the educational attainment of cohorts born in a short window from 1970 to around 1976. The changes allowed more 18-year olds to receive higher education and led to around a 1.5-year increase in average years of schooling within one decade, therefore affecting both those who might have left school at the minimum school leaving age of 16 and those who progressed to finishing secondary school but who would not, before the reform, have entered tertiary education. Whilst this expansion is not as clean as a compulsory increase in the minimum school leaving age, it allows us to examine the relationship between an increase in education across a larger part of the educational attainment distribution than school leaving age reforms which affect only individuals at the lower end of the education distribution. This second set of reforms affects individuals born from around 1970 to 1976 who are now entering their 40s, at time when chronic conditions can begin to manifest themselves.
Both approaches require large samples to enable us to isolate the effect of an increase in education. We use data from a large nationally representative sample (the Quarterly Labour Force Survey) which contains around 5 million observations for the relevant years. To isolate causal effects, we use short time windows round the reforms to close down any effect of time-varying changes that affect both education and health. This gives us estimation samples of around 360,000 observations for the first reform, and around 425,000 observations for the second reform.1
For the first reform, we observe individuals in the relevant birth cohorts between the ages of 41 and 61, of whom 36% report having (at least) one chronic health condition. For the second reform, we observe individuals between the ages of 30 and 50, of whom 27% report having (at least) one chronic health condition. Our analysis focuses on whether an individual has any chronic condition, the number of these, and whether they have any of five important sets of conditions. These are cardiovascular diseases and diabetes, musculoskeletal conditions, neurological and sensory conditions, mental illness and, for the younger group affected by the educational expansion, respiratory conditions. These conditions, after minor illnesses such as the common cold, are the most common reason for workplace sickness absence. Mental illness alone accounts for nearly 12% of working days lost each year in the UK and is the largest single cause of disability in most developed countries.
We find that for individuals affected by both reforms, there is a clear, statistically significant negative association between years of education and chronic ill health, as expected. However, the strength of any association weakens considerably once we apply causal identification techniques. We show this statistically in our paper, but here show it in Figures 1 and 2.
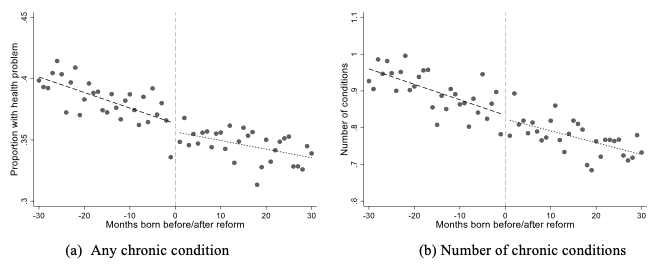
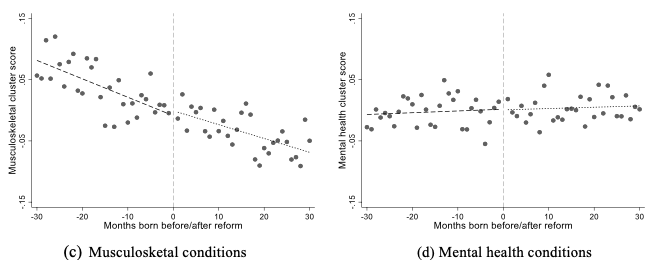
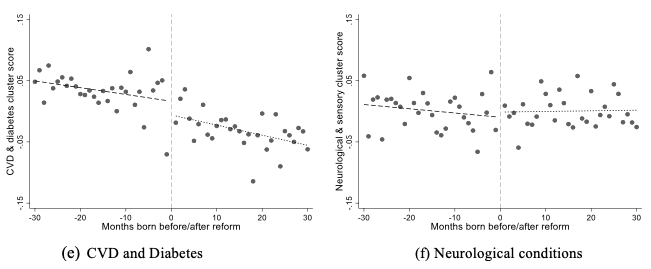
Figure 1 examines those affected by the 1972 reform. The figure plots the proportion of individuals with chronic health conditions by month of birth cohort within a 60-month window around the reform. The lines show before and after the reform date linear predictions. Evidence of a causal effect would show as a discontinuity around the reform date. Whilst there is possibly some indication of a discontinuity at the reform date for reporting any chronic health, shown in panel (a), there is no such relationship in any of the other panels except panel (e), which shows the cardiovascular and diabetes cluster of conditions. In contrast, we see no clear break for the number of conditions, musculoskeletal conditions, mental health conditions, or neurological and sensory conditions.
Figure 1 Prevalence of chronic conditions for months-of-birth around the 1972 reform cut-off
Notes: Each point represents the sample mean for a month-year of birth. Linear regression predictions from month of birth are calculated separately for months before and after reform.
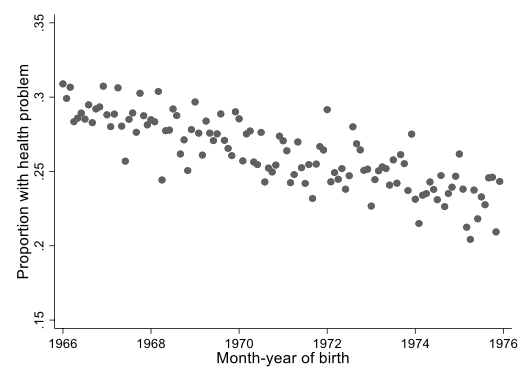
Figure 2 shows the incidence of any condition for those affected by the educational expansion. Again, there is no clear sign of a break – the incidence just declines gradually with age. Thus, this preliminary evidence suggests little causal relationship.
Figure 2 Prevalence of chronic conditions for months-of-birth around the education expansion reform
Note: Each point represents the sample mean for a month-year of birth.
Our statistical estimates confirm these patterns. For both reforms, there appears to be no statistically significant effect of an extra year of education on having a chronic condition, the number of conditions, or on most of the broad sets of conditions we examine. However, there is one exception to this. For the cardiovascular and diabetes cluster of conditions education appears to be protective, both for the older cohort affected by the raising of the minimum school age and for the younger cohort who experienced a more general increase in educational attainment. This appears to be driven by the incidence of diabetes. The estimated protective impact of education is larger for the older cohort, which is probably due to the fact that diabetes emerges over time and thus has a greater incidence at older ages. Our estimates suggest that an extra year of education reduces the probability of having diabetes by 3.6 percentage points (relative to a mean of 4% in the sample) for the older sample affected by the school age reform. For the younger sample affected by the educational expansions, the effect is to decrease the incidence of diabetes by 0.9 percentage points (relative to a mean of 1.8%).
We draw two takeaways. First, even with the largest survey sample available for the UK, the level of precision we can achieve means that, at the most conservative, we cannot rule out some potential educational effects, positive or negative. Second, even with this caveat, only for self-reported diabetes do we find statistically significant evidence that an extra year of education has a beneficial effect on health. This finding is intriguing. It chimes with the attempts to use educational programmes to reduce the incidence of diabetes in many developed countries, but many of these have not been evaluated robustly. Our findings draw attention to the need to examine the paths by which education causally affects the onset and management of diabetes. They also demonstrate that to implement the robust estimation methods required for policy evidence on the link between education and chronic health conditions will require very large samples.
References
Bedard, K and O Deschênes (2006), “The long-term impact of military service on health: Evidence from World War II and Korean War veterans”, American Economic Review 96: 176-194.
Clark, D and H Royer (2013), “The effect of education on adult health and mortality: Evidence from Britain”, American Economic Review 103: 2087-2120.
Davies, N, M Dickson, G Davey Smith, G van den Berg and F Windmeijer (2018), “The causal effects of education on health outcomes in the UK Biobank”, Nature Human Behaviour 2: 117-125.
Galama, T, A Lleras-Muney and H van Kippersluis (2018), “The effect of education on health and mortality: A review of experimental and quasi-experimental evidence”, NBER Working Paper 24225.
Hamad, R, H Elser, D C Tran, D H Rehkopf and S N Goodman (2018), “How and why studies disagree about the effects of education on health: A systematic review and meta-analysis of studies of compulsory schooling laws”, Social Science and Medicine 212: 168-178.
Janke, K, D Johnston, C Propper and M Shields (2020), “The causal impact of education on chronic health: Evidence from the UK”, Journal of Health Economics 70.
Lleras-Muney, A (2005), “The relationship between education and adult mortality in the United States”, Review of Economic Studies 72: 189-221.
Meghir, C, M Palme and E Simeonova (2018), “Education and mortality: Evidence from a social experiment”, American Economics Journal: Applied Economics 10: 234-256.
Oreopoulos, P (2006), “Estimating average and local average treatment effects of education when compulsory schooling laws really matter”, American Economic Review 96: 152-175.
Endnotes
[1] To derive causal estimates for the 1972 reform we follow Clark and Royer (2013) and use a conservative fuzzy regression discontinuity approach, with a tight 30-month bandwidth around this reform to close down the effect of time-varying changes that affect both education and health. Identification from the second reform is less straightforward but we use an estimation strategy in which identification comes from across cohort covariation in education and chronic health conditions (Bedard and Deschênes 2006).