A transplant is a life-saving treatment for patients with kidney failure. Unfortunately, most patients will never receive a transplant because there is a severe shortage of kidneys. The waiting list for deceased donor kidneys now exceeds 100,000 patients. Some patients are lucky enough to receive donations from living donors: friends, relatives, and rare Good Samaritan donors (Matthews 2017).
But many patients who have a potential living donor cannot receive a transplant directly because they may not be biologically compatible. These incompatibilities occur because of blood type and because of the patient’s immune response to the donor’s proteins. Many patients with a willing donor remain unmatched because of biological compatibility.
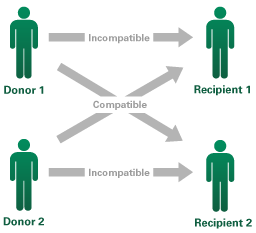
Kidney exchange is an innovative way to increase transplants. The idea is to find exchanges between pairs of patients and donors (Roth et al. 2004). For example, suppose Alice is willing to donate a kidney to Ben but is incompatible; and Charlie and Debbie are in an identical position. However, it may be possible to transplant Alice’s kidney to Debbie and Charlie’s kidney to Ben (see Figure 1). Such a two-way swap enables both patients to receive a transplant, with each patient’s related donor only donating one of their kidneys.
Figure 1 Two-way kidney exchanges
Although Donor 1 is willing to donate a kidney to Recipient 1, and Donor 2 to Recipient 2, they are incompatible. However, it may be possible to transplant Donor 1’s kidney to Recipient 2, and Donor 2’s to Recipient 1.
This basic principle has been extended to three-way swaps and even a six-way swap.1 Good Samaritan donors can also enable kidney chains, where each donates a kidney to a stranger, to transplant many more patients.2
Figure 2 A three-way exchange is also possible, extending the basic principle of the two-way exchange
Source: UAB News,The University of Alabama at Birmingham.
From 2008 to 2014, kidney exchange has grown from 300 transplants per year to 800 transplants per year. The system grew from one-off arrangements made by individual doctors or hospitals that were treating many patients, to a small consortia of hospitals, and finally to national kidney exchange platforms. These platforms use systematic computer algorithms that are able to find more complicated arrangements, such as kidney chains and three-way or four-way swaps. The algorithms are most powerful when a large number of patients and donors are all registered on the same system.
This evolution and growth of kidney exchanges have resulted from a mix of practical experimentation and academic studies. Medical doctors, economists, and researchers from various disciplines were involved with the creation of some of the first large kidney exchange platforms, and continue to work towards finding ways to better match patients and donors (Shute 2015, Roth et al. 2007, Rees et al. 2009, Anderson et al. 2015). By 2014, the national platforms were responsible for about 400 transplants per year.
The impact of market fragmentation
In a recent study we found that, despite the growth of these national kidney exchange platforms, the majority of kidney exchanges continue to be performed within hospitals (Agarwal et al. 2018). Hospitals only sign up a fraction of their patients with national kidney exchange platforms, while many hospitals do not participate in any of the national platforms. And, even among most hospitals that do participate, kidney exchanges tend to be performed internally.
The evidence suggests that not only is the market fragmented, but this fragmentation has a large efficiency cost that reduces the total number of transplants performed. National platforms, because of their size, can find more transplant possibilities and therefore match a greater fraction of patients than any single hospital can.
- First, we found that hospitals conducting their own matches are more likely to perform inefficient matches. For example, models show that it is almost never optimal to transplant a blood-type-O donor to a patient that does not have blood type O in a kidney exchange. This is because a blood-type-O donor is universally blood-type compatible and his or her organ can usually be used to set up a larger cycle or chain. Yet, individual hospitals are two to four times more likely to perform this type of inefficient transplant than national platforms.
- Second, we used detailed data on transplants and knowledge of the matching algorithms to estimate how size influences the ability of a hospital or platform to perform kidney exchanges. We found that individual hospitals are too small to perform efficiently. According to our estimates, improving the matching via coordination through the large national platforms can increase the total number of kidney exchange transplants by 25-55%. This corresponds to a waste of 200-440 transplants per year.
Policy implications
From a policy perspective, these findings suggest that we need to understand the reasons why hospitals do not participate more in national platforms, and design policies to increase participation.
There are two primary reasons why hospitals do not fully participate in kidney exchange platforms:
- First, current platform rules give incentives for hospitals to hoard easy-to-match patients and donors. Using these easy-to-match patients and donors in internal exchanges can often help the hospitals transplant other patients, while submitting them to a national platform may leave these patients un-transplanted. But registering the easy-to-match patients and donors brings a greater benefit to the kidney exchange system as a whole. Thus, current platform rules often put the hospitals in the difficult position of having to choose between helping their own patients or doing what is bestfor the system as a whole.
- Second, hospitals have to incur unreimbursed costs of participating in kidney exchange platforms. These include hiring additional transplant coordinators, performing additional medical tests, and paying platform fees. These costs are not covered by Medicare or insurance companies and can be a barrier to participating in kidney exchange platforms, particularly for small hospitals.
Both of these problems can be fixed using simple policies. Redesigning platforms with an eye towards encouraging full participation can alleviate the first problem. The platform can prioritize patients at hospitals that register altruistic donors as well as their easiest-to-match patients and donors, which could encourage hospitals to register those patients. These easy-to-match patients and donors are essential in arranging kidney exchanges. For example, altruistic donors are necessary for starting kidney chains that enable transplants for many patients. Hospitals should be encouraged to register altruistic donors at national platforms, which can set up long kidney chains.
Fixing the second barrier calls for reimbursement reform, both at the federal level and at the individual insurer level. This concern has been voiced by researchers and by the medical profession as well, who have proposed ways in which to alleviate this problem (Rees et al. 2012).
These lessons may be applied more broadly. Most European countries that have a national kidney exchange platform require full participation and do not face this free-riding problem (possibly due to the structure of the health system). However, each of these platforms is small and some countries, such as Austria and the Czech Republic, and Italy, Spain, and Portugal, have been trying to combine their platforms. Just like some hospitals do in the United States, these countries have so far shared only the patients and donors that they cannot match internally, leading to poor results. The results from this study can explain some of the challenges and potential solutions in this endeavour.
There are many other approaches currently being explored to expand kidney exchange, and make it a more effective tool so that patients currently waiting for a kidney can get a transplant. One idea, proposed by researchers at Boston College, is to find ways in which all kidney patients with living donors are incentivised to participate in kidney exchanges by utilizing the deceased donor pool (Sönmez et al. 2017). Another proposal is to use kidneys from deceased donors to initiate kidney chains (Haynes and Leishman 2017). These innovations hold the promise of vastly expanding the number of kidney transplants that may be possible.
References
Agarwal, N, I Ashlagi, E Azevedo, CR Featherstone, Ö Karaduman (2018), “Market failure in kidney exchange”, NBER Working Paper No. 24775.
Anderson, R, I Ashlagi, D Gamarnik and AE Roth (2015), “Finding long chains in kidney exchange using the travelingsalesman problem”, PNAS 112(3): 663-668.
CBS News (2018), “Patients of six-way kidney swap meet for the first time”, video, 20 January 2018.
Matthews, D (2017), “Why I gave my kidney to a stranger — and why you should consider doing it too”, Vox.com, 11 April.
Pope, A (2018), “Nation’s longest single-site kidney chain passes 100”, Alabama Newscenter, 19 August.
Rees, MA, JE Kopke, RP Pelletier, DL Segev, ME Rutter, AJ Fabrega, J Rogers, OG Pankewycz, J Hiller, AE Roth, T Sandholm, MU Ünver, et al. (2009), “A nonsimultaneous, extended, altruistic-donor chain”, New England Journal of Medicine 360:1096-1101.
Rees, MA, MA Schnitzler, EY Zavala, JA Cutler, AE Roth, FD Irwin, SW Crawford, AB Leichtman (2012), “Call to develop a standard acquisition charge model for kidney paired donation”, American Journal of Transplantation 12(6): 1392-7.
Roth, AE, T Sönmez and MU Ünver (2004), “Kidney exchange”, The Quarterly Journal of Economics 119(2): 457–488.
Roth, AE, T Sönmez and MU Ünver (2007), “Efficient kidney exchange: Coincidence of wants in markets with compatibility-based preferences”, American Economic Review 97(3): 828-851.
Shute, N (2015), “How an economist helped patients find the right kidney donors”, NPR, 11 June 2015
Sönmez T, U Unver and MB Yenmez (2017), “Incentivized kidney exchange”, Boston College Working Papers in Economics 931 (revised 2018).
Haynes, CR, and R Leishman (2017), “Allowing deceased donor-initiated kidney paired donation (KPD) chains”, OPTN/UNOS Kidney Transplantation Committee, concept paper.
Endnotes
1 See https://www.cbsnews.com/video/patients-of-six-way-kidney-swap-meet-for-the-first-time/
2 See https://www.alabamanewscenter.com/2018/08/19/nations-longest-single-site-kidney-chain-reaches-100/