Poorer people have worse health at birth, are sicker in adulthood, and die younger than richer people. Indeed, growing evidence across various disciplines reveals stark correlations between health capital and socioeconomic status (e.g. Marmot et al. 1991, Case et al. 2002, Deaton 2002, Currie 2009, Lleras-Muney 2018).
Yet, the mechanisms underlying these associations are poorly understood. Several proposed explanations suggest that individuals growing up in poor households make fewer investments into their health throughout their lifetime, albeit we do not know why that is the case.
In a recent paper, we ask whether unequal access to informal health expertise contributes to health inequality (Chen et al. 2019). The overwhelming share of individuals’ decisions about their own health investments happens outside of the walls of the formal healthcare system. If, from a very young age, children in poorer households are exposed to less health-related expertise, and, as a result, acquire less tacit knowledge about how to invest in their health, then we would expect these children to have worse health and higher mortality as adults.
Thus, our hypothesis is that exposure to informal health expertise affects health, and, consequently, that unequal access to such expertise may perpetuate differences in health between richer and poorer households. To test this hypothesis empirically, we consider one quantifiable measure of exposure to informal health expertise: having a health professional – a medical doctor or a nurse – in the family.
For our analysis, we use rich administrative data from Sweden. These data include rich socioeconomic information, precise information about education, detailed birth records, health care records, and prescription drug records, and mappings of family trees spanning four generations.
Despite Sweden’s universal health insurance system and generous social safety net, we document pronounced inequality in mortality and morbidity. For example, out of 100 individuals that are alive at age 55, nearly 45 will have died by age 80 at the bottom of the income distribution (lowest 5%), while fewer than 25 will have died among the top 5%. We find similarly large differences in the prevalence of lifestyle-related chronic conditions at older ages, in the rate of preventive investments among adolescents, and in the rate of prenatal tobacco exposure. Hence, despite equalised formal access to healthcare and a well-developed social safety net, Sweden exhibits substantial health inequality, measured across a wide range of ages and conditions. In fact, we find that at age 75, mortality inequality is equally pronounced in Sweden as it is in the US.
These facts motivated us to examine a mechanism other than differences in health insurance or access to care that may perpetuate socioeconomic differences in health. Specifically, we ask whether a lifetime of differences in exposure to informal health expertise can account for some of the observed patterns of health inequality. Differences in the tacit knowledge of how to invest in one’s health, it seems, could persist even in an environment with universal health insurance and equal formal access to healthcare.
We start by comparing individuals who have a doctor or a nurse in the family to observationally similar individuals who do not. We find that individuals with relatives in the health profession are 10% more likely to live beyond age 80. They are also significantly less likely to have chronic lifestyle-related conditions, such as heart attacks, heart failure, and diabetes. Younger relatives within the health professional’s extended family also see gains: they are more likely to get vaccinated, have fewer hospital admissions, and have a lower prevalence of drug or alcohol addiction. In addition, the closer the relatives are to their familial medical source—either geographically or within the family tree—the more pronounced are the health benefits, according to our findings.
Naturally, we may be concerned that families with a nurse or a doctor are simply different from other families in some ways we cannot observe. These families may talk more about health, may have healthier habits, and may make larger preventive health investments, for example. In a nutshell, they may both be healthier and have a health professional in the family because of their interest in health—rather than the other way around.
To overcome this and to quantify the role of informal exposure to health expertise via a medical professional in the family, while avoiding results that would be muddled with other differences between individuals with and without a doctor in the family, we use two different empirical approaches.
First, we take advantage of the fact that in some years and for some sets of applicants, randomisation was used to break ties among equally qualified applicants to Sweden’s medical schools. This allows us to use medical school application records and compare the health of family members of applicants who won and lost such ‘lotteries’ (applicants can reapply, so we use the lottery outcome on an applicant’s first admission attempt). We find that having a relative matriculate into medicine reduces older individuals’ risk of heart attack and heart disease, raises preventive investments and adherence to cardiovascular medication, and generally improves health. All these effects are measured over a period of 6 to 8 years from the relative’s matriculation into medical school. Younger generations also benefit from having a relative get medical training: they make larger preventive investments, are more likely to get vaccinated, and have fewer hospital admissions and addiction cases.
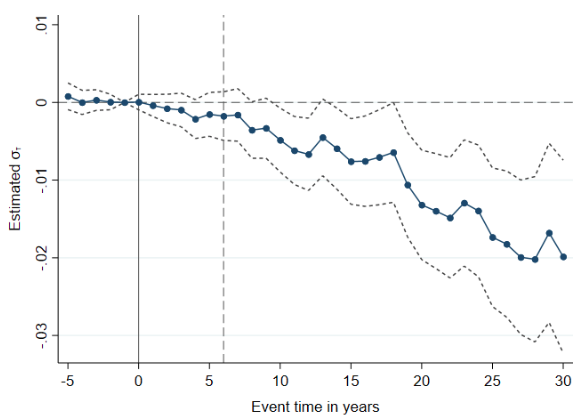
Second, we examine long-run outcomes by comparing mortality and the prevalence of chronic conditions in the extended families of individuals who train as medical doctors and lawyers, respectively. While both professions enjoy similar levels of income and social status, doctors have a higher degree of health expertise that they can transmit to their families. Comparing more than 30 years of detailed health records, we find that family members of doctors are 10% more likely to be alive than family members of lawyers 25 years after their younger family member matriculated in medical or law studies (see Figure 1). The relatives of doctors also faced lower prospects of lifestyle-related chronic diseases.
Figure 1 Doctor in the family and long-run mortality: Event study
Notes: The figure illustrates the impact of having a family member trained as a physician (relative to having a family member trained as a lawyer) on the probability of death, along with 95% confidence intervals. The regressions are centred at event year -1, i.e. 1 year before the year of matriculation in a medical (or legal) degree. The dashed vertical line marks the average graduation time for physicians. Standard errors are clustered at the family level. The estimates reveal a clear slowdown in the relative mortality rate among relatives of doctors (as compared to the relatives of lawyers) that starts emerging around year 8 after the young relative matriculates into college. The mortality gap then steadily widens for two decades. The point estimates suggest a 1.7-percentage-point decrease in the probability of death by event time 25, which corresponds to a 10% decline off the mean among relatives of lawyers, which is 17%. The sample includes family members born in Sweden between 1936 and 1940. We exclude family members who are themselves a health professional or have a health professional spouse.
An explanation that is commonly discussed in policy circles for the existence and persistence of a negative correlation between socioeconomic status and health is differences in access to healthcare across the socioeconomic spectrum. Our evidence suggests that this explanation can only be one piece of the health inequality puzzle. What’s more, our results imply that a scarcity of access to expertise in households at the lower rungs of the socioeconomic ladder can create and sustain inequality in health outcomes—even in an environment with fully equalised access to formal healthcare, generous social insurance programs, and a wide social safety net.
It is encouraging, however, that the benefits accruing to medical professionals’ family members appear to be scalable. Our analysis suggests that access to expertise improves health not through preferential treatment, but rather through intra-family transmission of ‘low-tech’ (and hence, cheap) determinants of health, likely ranging from the sharing of nuanced knowledge about healthy behaviours to reminders about adherence to chronic medication, and to frequent and trustful communication about existing health. This implies that public health policies, as well as carefully designed public and private health insurance contracts that successfully mimic intra-family transmission of health-related expertise, would have the potential to close a significant share—our estimates suggest as much as 18%—of the income-mortality gap.
References
Case, A, D Lubotsky and C Paxson (2002), “Economic status and health in childhood: The origins of the gradient”, American Economic Review 92(5): 1308–1334.
Chen, Y, P Persson and M Polyakova (2019), “The roots of health inequality and the value of intra-family expertise”, CEPR Discussion Paper 13583.
Currie, J (2009), “Healthy, wealthy, and wise: Socioeconomic status, poor health in childhood, and human capital development”, Journal of Economic Literature 47(1): 87–122.
Deaton, A (2002), “Policy implications of the gradient of health and wealth”, Health Affairs 21(2): 13–30.
Lleras-Muney, A (2018), “Mind the gap: A review of the health gap: The challenge of an unequal world by Sir Michael Marmot”, Journal of Economic Literature 56(3): 1080–1101.
Marmot, M G, S Stansfeld, C Patel, F North, J Head, I White, E Brunner, A Feeney and G Davey Smith (1991), “Health inequalities among British civil servants: The Whitehall II study”, The Lancet 337(8754): 1387–1393.