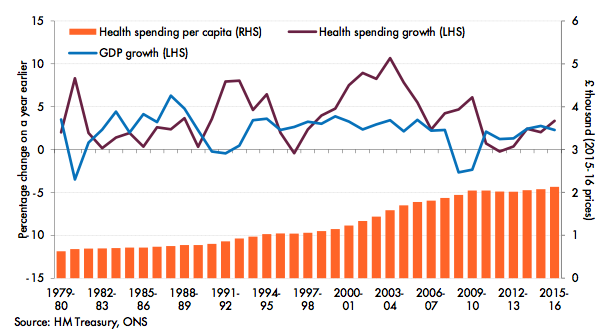
Many domestic and international studies foresee upward pressure on healthcare spending as one of the greatest challenges to long-term fiscal sustainability. Evidence from the UK (common to other countries) is that health spending has grown faster than the economy over time. In real terms, public spending on health has increased by 3.8% a year on average since 1978-79, while the economy has grown by an average of just 2.2% per year. In real per capita terms, health spending has also increased steadily over time (Figure 1). Population ageing – a commonly cited driver of health spending – cannot on its own account for this increase.
Figure 1. Year-on-year increases in real health spending and GDP in the UK
Demographic factors
Demographic change is a key long-term pressure on the public finances. Like many developed nations, the UK’s population is projected to age over the next few decades, with the ‘old-age dependency ratio’ – the ratio of the elderly to those of working age – rising. This reflects increasing life expectancy (particularly among older people), relatively low fertility rates, and baby-boomer cohorts retiring.
Morbidity – life expectancy spent in ill health – is an associated demographic driver of health spending. More years spent in ill health (expansion of morbidity) – for example, if medical technology becomes better at preventing fatal outcomes without altering the underlying prevalence and progression of the disease – increases pressure on health spending. More years spent in good health (compression of morbidity) – for example, thanks to new medical technologies that slow the progression of chronic diseases – might raise GDP by more than any age-related increase in health spending.
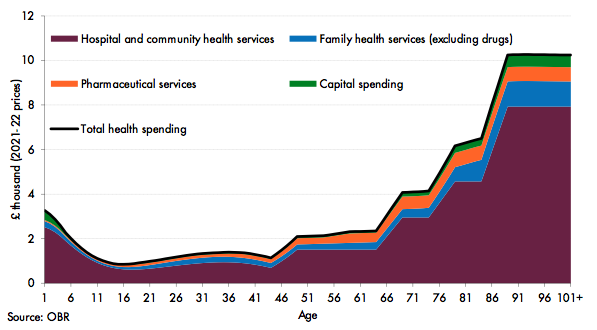
We model health spending using representative profiles for age-related health spending (Figure 2). These assume that health spending per person is relatively high in early age due to the costs associated with birth and other childhood health needs, such as vaccinations. It is then low during working age before increasing substantially later in life. As a result, unless rising life expectancy is accompanied by more years spent in good health, an ageing population would be expected to raise average health spending per capita, and thus both total health spending and spending as a share of GDP. The Office for Budgetary Responsibility’s (OBR) projections now assume that increases in life expectancy are split evenly between time in good and ill health (Licchetta and Stelmach 2016).
Figure 2. Representative profile for health spending
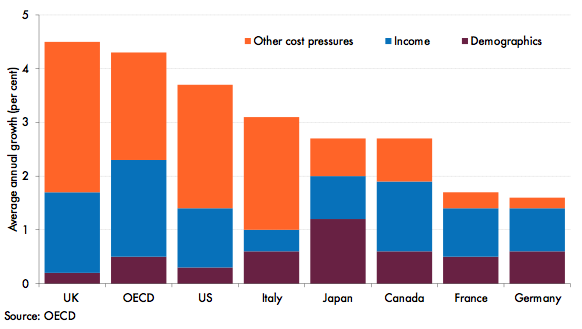
Empirical studies have tended to find relatively small effects of ageing on health spending. For example, Figure 3 shows that real public health spending per capita in OECD countries between 1995 and 2009 was mainly driven by rises in income and other non-demographic drivers, rather than demographic effects (De la Maisonneuve and Oliveira Martins 2013).
Figure 3. Growth in public health spending per capita (1995-2009)
Income effects
Healthcare is generally seen as a ‘normal good’, which means that people tend to demand more of it as their incomes rise. This means that spending rises in cash and real terms as incomes rise, but whether spending rises or falls as a share of GDP depends on whether the ‘income elasticity of demand’ is greater or less than one.
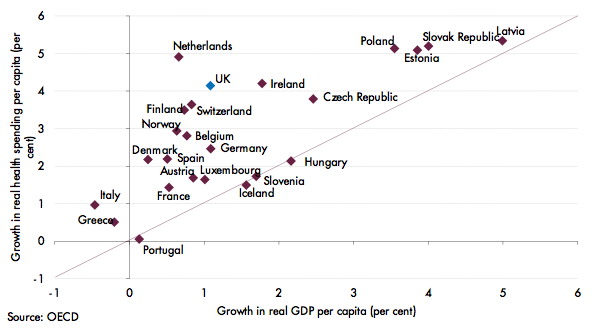
Figure 4 shows that health spending has risen faster than GDP in almost all European countries since 2000. Most agree that the relationship between per capita health spending and GDP in OECD countries is positive – that the income elasticity of health spending is above zero – but there is no consensus on the size of the elasticity. That disagreement partly relates to how much spending growth researchers assign to the income elasticity or to other cost pressures.
Figure 4. Growth of real health spending and GDP per capita (2000 to 2015)
Other cost pressures
Other cost pressures cover many factors. Key among them are increasing relative healthcare costs (e.g. reflecting lower productivity growth in healthcare than the rest of the economy), the effect of technological advances (e.g. medical equipment, techniques, and procedures), and the rise of chronic conditions.
Healthcare provision is relatively labour intensive. For example, the King’s Fund found that staff accounted for around 70% of a typical hospital’s total costs and that this proportion had risen over time (Appleby et al 2014). So we might expect productivity growth to be slower in this sector than in the economy as a whole. Indeed, available estimates suggest that healthcare productivity has risen by about 1.2% a year on average between 1979 and 2014 compared to 1.8% in the whole economy. According to the so-called ‘Baumol cost disease’ theory, real wages in the healthcare sector must keep pace with the rest of the economy in order to attract and retain staff, but slower productivity growth means that additional input would be needed to achieve a desired increase in care per person (Baumol and Bowen 1966).
Exposure to new or better technologies can improve healthy life expectancy but, unlike in other industries, technological innovations in healthcare have generally been cost-escalating rather than cost-containing. Different studies attribute between 27 and 75% of growth in health spending in advanced economies to technological change (European Commission 2015, Congressional Budget Office 2008). New technologies often treat conditions for which there was previously no, or no effective, treatment (e.g. renal dialysis and coronary artery bypass grafts) or expand existing methods to wider patient populations (known as ‘treatment expansion’). Even if an advance reduces the cost of treatment, spending can increase if that treatment finds wider medical uses and hence addresses unmet demand for care.
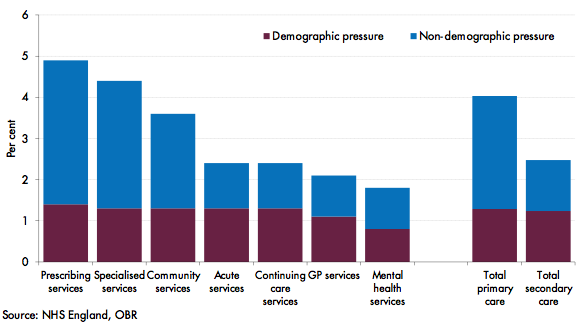
NHS England (2016) estimated non-demographic cost growth pressures for the NHS up to 2020-21 by stripping out an estimate of demographic cost pressures from activity in 2015-16 (Figure 5). This suggests that, on average in 2015-16, other cost pressures added 2.7 and 1.2 percentage points to growth in primary and secondary care spending respectively. The size of the effect varies significantly by spending category, being particularly large for prescribing and specialised services. By contrast, demographic factors are similar across most services, contributing on average around 1.3 percentage points to growth in total activity.
Figure 5. Demographic and non-demographic pressures (2015-16)
Implications for the OBR’s long-term fiscal projections
The OBR’s long-term fiscal projections did not include explicit adjustments for other cost pressures in the health sector until this year. In order to include other cost pressures in the long-term spending projections, we used the NHS England estimate for non-demographic cost pressures in 2015-16 as the starting point, then assumed that these pressures will decline over time – as might be expected as health spending takes up an ever larger share of national income. Specifically, we assumed a linear convergence for both primary and secondary care to a 1% a year increase from 2036-37 onwards. (This is the same steady-state growth rate used by the US Congressional Budget Office when considering the average excess cost growth over the past 30 years and the flexibility to restrain costs in the future.)
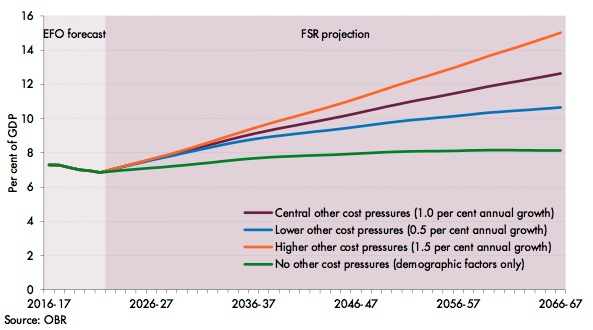
Including other cost pressures had a significant effect on the health spending projection presented in the 2017 Fiscal sustainability report (Office for Budget Responsibility 2017). Figure 6 shows spending on health rising from 7.3% of GDP in 2016-17 to 12.6% of GDP in 2066-67. This was around 4.6% of GDP higher than the 2015 projection, of which 4.5% of GDP reflected the new assumption about additional cost pressures. Faster or slower other cost pressure would see health spending rise by more or less than in our central projection.
Figure 6. Healthcare spending under alternative other cost pressure assumptions
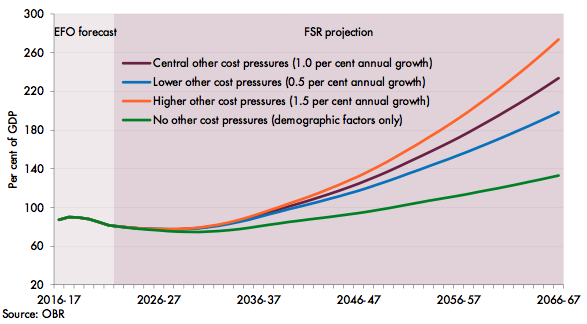
The inclusion of other cost pressures in the long-term health spending projection also accounted for the majority of the increase in public sector net debt by 2066-67. Excluding the effect of these cost pressures, public debt would have reached 133% of GDP by 2066-67, some 101% of GDP below the central projection that included the extra pressures on health spending (Figure 7).
Figure 7. Sensitivity of net debt projections to health-specific assumptions
Similar to health spending, the debt projections are very sensitive to assumptions about the pace at which non-demographic cost pressures push health spending up. But under the current policy setting, all scenarios point to significant upward pressure from non-demographic drivers of spending. That would require larger fiscal adjustments to bring public debt more in line with pre-crisis levels.
References
Appleby, J, A Galea and R Murray (2014) The NHS productivity challenge, The King’s Fund, May.
Baumol, W and W Bowen (1966) Performing arts: The economic dilemma, New York: The Twentieth Century Fund.
Congressional Budget Office (2008) “Technological change and the growth of health care spending”, January.
De la Maisonneuve, C and J Oliveira Martins (2013) “A projection method for public health and long-term care expenditures”, OECD, Economics Department Working Papers No 1048, June.
European Commission (2015) “The 2015 Ageing Report: Economic and budgetary projections for the 28 EU Member States (2013-2060)”, European Economy, 3, May.
Licchetta, M and M Stelmach (2016) “Fiscal sustainability and public spending on health”, Office for Budget Responsibility Working Paper No 9, September.
NHS England (2016) NHS five year forward view: Recap briefing for the Health Select Committee, May.
Office for Budget Responsibility (2017) Fiscal sustainability report, January.